I don’t have any information about the patient, but can you provide a full description of the rhythm on this 3-lead recording?
Recent News Posts
- AHCS Accredited Specialist Echocardiography Register is NOW OPEN 14/10/2024
- Dr Richleys ECG of the Month – October 2024 01/10/2024
- Revised Standards: recording and reporting 12-lead electrocardiograms 30/09/2024
- Invitation to Tender for SCST Administration Services 12/09/2024
- Dr Richleys ECG of the Month – September 2024 01/09/2024
Recent Comments
- Dave Richley on Dr Richleys ECG of the Month – October 2024
- Tenisha De Coteau on Dr Richleys ECG of the Month – October 2024
- Dave Richley on Dr Richleys ECG of the Month – October 2024
- Ōkóyè Ō. on Dr Richleys ECG of the Month – October 2024
- Dave Richley on Dr Richleys ECG of the Month – October 2024

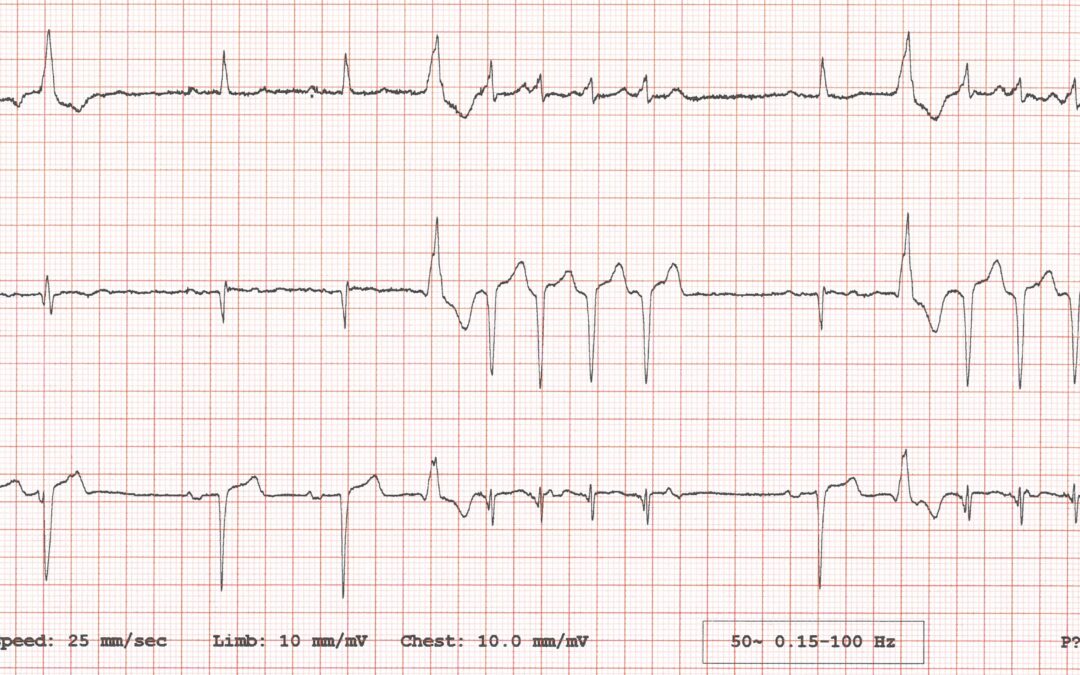
Sinus rhythm, first degree AV-block (PR ~220ms), with marked Q-waves in lead III (possible old inferior MI – deep inspiration please).
Sinus P-wave rate is unchanged by ectopic beats, therefore we have no V-A conduction.
I believe the short runs are deceptively broad, appearing narrow, but actually measure ~120ms in lead II.
These short runs appear to be triggered by a distinctly different ventricular ectopic complex and could be caused by a Ventriculo-Hisian accessory pathway initiating a short self-limiting re-entrant arrhythmia.
As Scott says, this ECG seems to show sinus rhythm with 1st degree AV block and short runs of ventricular premature beats. I agree with him that the sinus rate is unchanged by the VPBs – I can make out dissociated sinus P waves throughout the ventricular ectopic activity. I also agree with Scott that although the premature complexes may appear narrow at first glance, they are actually 120 ms in duration when measured in lead II. Scott suggests that the ectopic runs may be reentrant in nature, initiated by the 1st VPB and involving a ventricular-Hisian accessory pathway. I must confess that this is beyond my level of knowledge – do any of SCST’s EP/arrhythmia experts have any comments to offer on this theory?
One thing I disagree with Scott about is the usefulness of recording lead III on deep inspiration to determine whether or not the Q wave is pathological. I know this is standard practice in some departments but several studies back in the 1970s (1,2,3) failed to find any benefit in this manoeuvre and as far as I know there are no authoritative recommendations for it. I’m happy to be corrected though! If there is not a pathological Q wave in aVF (>25% of the R wave amplitude), then a Q wave in lead III can be ignored.
References:
1. Shettiga UR, Hultgrenm HN, Pfeifer J, Lipton MJ (1974). Diagnostic value of Q-waves in inferior myocardial infarction. Am Heart J 88(3):170-175.
https://doi.org/10.1016/0002-8703(74)90006-4
2. Bodenheimer MM, Banka VS, Helfant RH (1977). Determination of lead III Q waves significance. Utility of deep inspiration. Arch Intern Med 137(4):437-9.
3. Mimbs JW, deMello V, Roberts R (1977). The effect of respiration on normal and abnormal Q waves. An electrocardiographic and vectorcardiographic analysis. Am Heart J 94(5):579-84.
If the lead III Q-wave confirms old MI then of course the ventricular runs may represent simple scar related re-entrant rhytms.
Sir any chance of turn into nsvt